Gluteal Tendinopathy: Managing Your Hip Pain
Gluteal tendinopathy has been called many a name over the years – trochanteric bursitis, gluteal bursitis, greater trochanteric pain syndrome – however, the pattern we see as clinicians is often very similar. That is, pain over the side of the hip with or without down the thigh, pain with lying on your side at night, pain in standing, walking, climbing up and down stairs. Between the ages of 50-70years old, gluteal tendinopathy afflicts approximately 24% of women, up to 4 times more women than men!
What is Gluteal Tendinopathy?
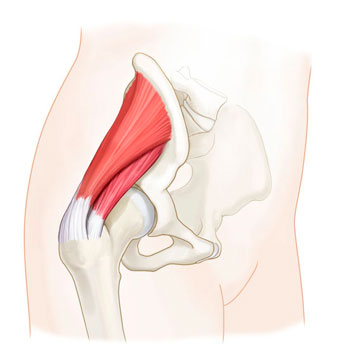
Gluteal tendinopathy is when there is thinning or tearing of the deep fibres of the gluteus medius and/or minimus muscle tendons, which sit under our large gluteus maximus muscle. These tendons attach to the greater trochanter the femur bone (the bony part on the side of the hip). Gluteal tendinopathy often occurs without any injury or sudden pain, instead pain tends slowly builds over time until it’s hard to walk and hard to sleep at night.
Is it Bursitis?
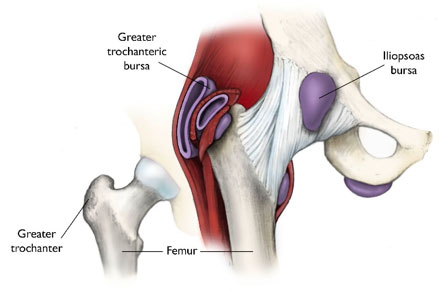
You may have heard the name gluteal or trochanteric bursitis before. Traditionally, it was thought inflammation of one or more of the bursae of the hip was the main driver of lateral hip pain. Bursa being small fluid sacs that help lubricate movement between muscles and bones. However, research shows this may be a minority of cases with only 20% of those with lateral hip pain having bursa irritation on medical imaging. Rather, it appears break down of gluteal tendon tissue is the culprit of lateral hip pain, lending the condition the name “Gluteal tendinopathy”.
Tendinopathy of the gluteus medius or minimus muscles happen with one of more of the following mechanisms:
1. LACK OF GLUTEAL STRENGTH AND WHICH PROTECTS TENDONS FROM OVERLOAD
The capacity of our deep gluteal muscles (medius and minimus) to bear load plays crucial role in the development of this condition. The role of tendon is to transmit force from the muscle to the bone or vice versa. When the muscle is weak it can become overloaded even in in non-strenuous activities, like walking, and as a consequence the tendon compensates by absorbing the excess load.
Problems arise as the tendon isn’t designed to absorb load, only transmit it. As such, tendon tissue begins to tear and break down, and eventually lead to the development of pain and tendinopathy.
2. COMPRESSIVE FORCES ON THE MUSCLE TENDONS FROM BONY ALIGNMENT
Tendon don’t like compression. Specifically the tendons of gluteus medius and minimus don’t like being compressed on the greater trochanter of the hip. Compression of these tendon over the bone prominence of the hip leads to irritation and can progress to tearing of its deep fibres.
Factors that develop how much compressive force is over the lateral hip can be boiled down to bone alignment, however there are two main aspects that affect bony alignment in Gluteal tendinopathy.
a) Poor pelvic stability leading to excessive adduction of the hip
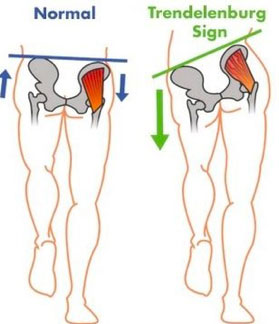
First, the pelvis makes the floor of our core system, and as such, in movement and mobility our pelvis is designed to remain level as our legs move around it. Problems arise if pelvis stability is poor as this leads to the development of a hip drop pattern or “Trendelenberg’s sign” in single leg activities, such as walking or getting in and out of the car. When this happens the superficial iliotibial band (ITB) which stretches the hip tightens and compresses the gluteal tendons underneath.
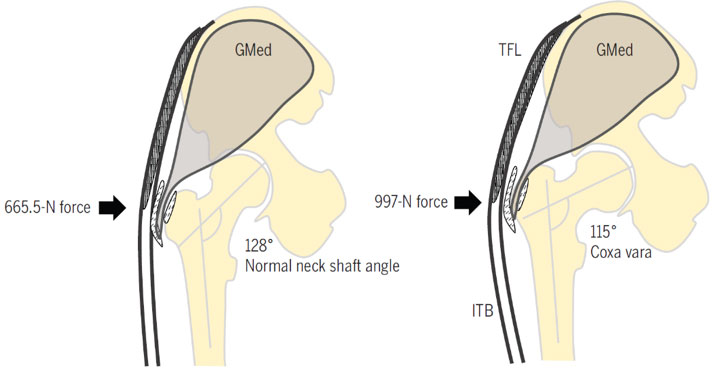
b) Angle of the femoral head compared to the femoral shaft
Second, the smaller the angle between the femoral head and the shaft, the greater the compressive load of the tendons on the hip as the ITB needs to stretch over it. Unfortunately a smaller angle or “coxa vara” is much more common in females, and this is something that we cannot change. This is why women with Gluteal tendinopathy outnumber men up to 4 times!
What Can We Do About It?
Good news is that gluteal tendinopathy is very fixable. Without resorting to surgical means, there are many options to relieve lateral hip pain. Short term improvement can be as simple as advice regarding activity modification, adaptive strategies, and postural correction. Small things including sleeping with a pillow between your legs, avoiding standing or sitting cross-legged can help to immediately reduce the compression on the hip and hence aggravation of the gluteal tendons. Furthermore, if there happens to be as aspect of bursitis or inflammation, your lateral hip pain may respond well to anti-inflammatory medication and possible cortisone injection later on.
Long term improvement comes from none other than a graded strengthening program. Strengthening the gluteal muscles helps to offload their respective tendons, hence break the cycle of overload and break down occurring in the tendon tissue. Some exercises to start may start with include:
- Clam exercises with resistance band, lying on back
- Glute bridges with resistance band or pillow between legs, lying on back
- Side-kicks in standing, with or without a resistance band
With tendinopathy, the tricky thing is exercise progression, making sure the exercises are challenging enough to cause tissue changes within the muscle-tendon complex but with minimal provocation of pain. In this regard, an exercise program guided by a health professional is often the gold standard in Gluteal tendinopathy treatment.

References:
1. Grimaldi A, Fearon A. Gluteal Tendinopathy: Integrating Pathomechanics and Clinical Features in Its Management. J Orthop Sports Phys Ther. 2015 Nov;45(11):910-22. doi: 10.2519/jospt.2015.5829. Epub 2015 Sep 17. Review. PubMed PMID: 26381486.