
Incontinence in the Female Athlete
Involuntary leakage, or Incontinence, is a topic that has been long over-looked in the domain of women’s health. Despite the fact that accidental leakage affects anywhere between 10-55% of us women between 15-60 years old(1). Even more so, those of us participating in sport are uniquely at risk, as the physical demand of our given sports increased the burden or load on the pelvic floor. About 30% of regular exercising women experience leakage in at one type of exercise(2).
What is Incontinence?
Incontinence is define as any involuntary leakage of urine, and can be one of 3 main types:
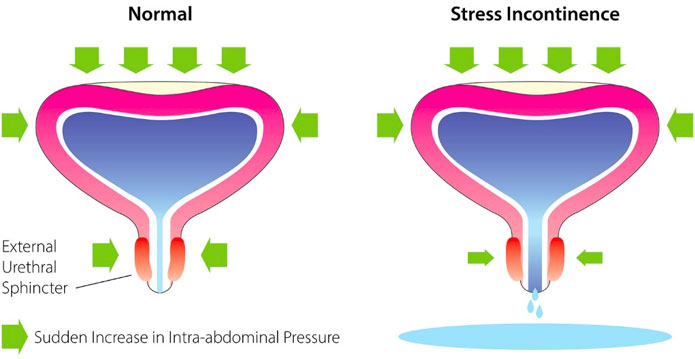
- Stress Incontinence: leakage on effort or exertion, such as sneezing, laughing or jumping
- Urgency Incontinence: leakage accompanied by a strong need to urinate
- Mixed Incontinence: a combination of both Stress and Urgency Incontinence
How Common Is It In Sport?
Although athletes of some sports are more prone to Urgency Incontinence, such as soccer or cycling(3), the vast majority of sportswomen will experience Stress Incontinence. Depending on the sport, Incontinence affects 28-80% of female athletes(4), with those most at risk being trampolinists, gymnasts, hockey players and ballet dancers, and any athlete participate in a jumping sport.
How Does Leakage Happen?
More specifically, Stress Incontinence occurs when there’s an increase in internal abdominal pressure, which is what happens when we laugh or jump or have to carry something heavy. As we “brace” our core this pushes down onto our pelvic floor, which sits like a sling supporting our bladder. Hence if our pelvic floor isn’t strong enough to counteract this downwards force, our bladder is squashed down and urine may leak out. In sports and exercise, we are constantly running, jumping, pushing, and pulling. And all this only helps to magnify the downwards pressure on our bladder and pelvic floor.
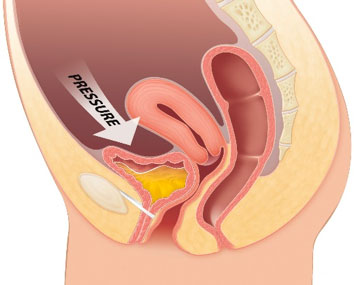
Adapted from Expert Chikitsa: Stress Incontinence
How Do We Fix Incontinence?
Good news is that nowadays there’s many an option to help accidental leakage, for the professional athlete or weekend warrior alike. First line, for almost all cases of Incontinence, is pelvic floor strengthening, under the direction of Physiotherapist or Women’s Health practitioner. Furthermore, depending on type of Incontinence, General practitioners can prescribe medications, supplements and assistive devices to help you get on with your life and the sport you love.
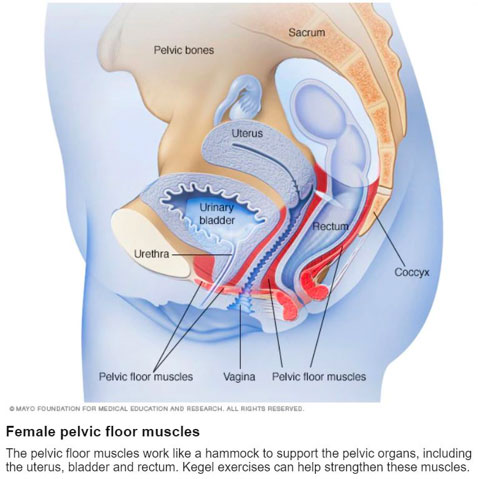
Activating our pelvic floor requires dedicated practice, but essentially it would feel like a slight “tighten and lift” sensation around your vagina. Activating your pelvic floor should feel like tightening to stop the flow of urine or holding onto wind. Once you’ve gotten the hang of this your Health Practitioner may progress you to learning to hold this contraction or coordinating it with movement, depending on when leakage happens for you.
References
1. Teixeira RV, Colla C, Sbruzzi G, Mallmann A, Paiva LL. Prevalence of urinary incontinence in female athletes: a systematic review with meta-analysis. Int Urogynecol J. 2018 Dec;29(12):1717-1725. doi: 10.1007/s00192-018-3651-1. Epub 2018 Apr 13. PubMed PMID: 29654349.
2. Nygaard I, DeLancey JO, Arnsdorf L, Murphy E. Exercise and incontinence.Obstet Gynecol. 1990 May;75(5):848-51. PubMed PMID: 2325968.
3. Townsend MK, Danforth KN, Rosner B, Curhan GC, Resnick NM, Grodstein F. Physical activity and incident urinary incontinence in middle-aged women. J Urol. 2008 Mar;179(3):1012-6; discussion 1016-7. doi: 10.1016/j.juro.2007.10.058. Epub 2008 Jan 18. PubMed PMID: 18206951; PubMed Central PMCID: PMC2712871.
4. Goldstick O, Constantini N. Urinary incontinence in physically active women and female athletes. Br J Sports Med. 2014 Feb;48(4):296-8. doi: 10.1136/bjsports-2012-091880. Epub 2013 May 18. Review. PubMed PMID: 23687004.